Background and purpose: coiling occlusion has been widely recommended as a standard treatment for cerebral aneurysm. However, the experience of this technique in Vietnam is still limited. We report the prospective case series of coiling occlusion at 2 military hospitals. We studied outcome, recurrence and complications of coiling occlusion for cerebral ruptured aneurysms.
Method: a prospective analysis of all patients with endovascular coil occlusion aneurysms collected from June 2008 to April 2011. Long-term follow - up angiograms for 36 months.
Results: There were 110 patients with 127 aneurysms. Clinical characteristics: severe headache 96.4%, nausea and vomiting 95.5%, consciousness disorder 65.5%, Warning leak 48,2%. Outcome (12 months after discharge): good 94.8%, bad 5.2%, death 8.4%. Re-bleeding 40%. Recurrence 13%.
Conclusion: coiling is an effective method to prevent the aneurysm from re-rupturing. The complications is acceptable and outcome is good.
Key Words: cerebral aneurysm; coiling occlusion
---------------------------------------------------------------------------
PATIENTS AND METHODS
Patients
One hundred and ten intra-cerebral hemorrhage patients because of aneurysms rupturing at hospital 103 and Military central hospital 108 from June 2008 to April 2011.
Methods
Prospective study with long-term observation
All patients were examine thoroughly according to case report template. We used Hunt-Hess scale to rate the severe of clinical manifestation. Rankin scale was used to rate outcome. We observed complications, especially re-ruptured
We applied CT (or MRI), MRA and DSA for every patients. We collected data about location, shape, size, neck-diameter of aneurysms.
After coiling embolization we used heparin 500UI/h in the first 48 hours, and then aspirin 100mg/24h PO. Patients were maintain their systolic blood pressure 150-160mmHg, the central venous pressure 8-12cm H2O, hematocrite 30-35%.
Re-examine and apply Angiographic follow-up at 3; 6; 12 and 36 months after treatment
We rated clinical state by Glasgow outcome scale: GOS IV-V = good; II-III = bad; I = death.
Statistic: we used SPSS 15.0
RESULTS AND COMMENT
Patients’ demographics
One hundred and ten patients were studied, their age from 27 to 79 year-old. Male/female 1.5/1.
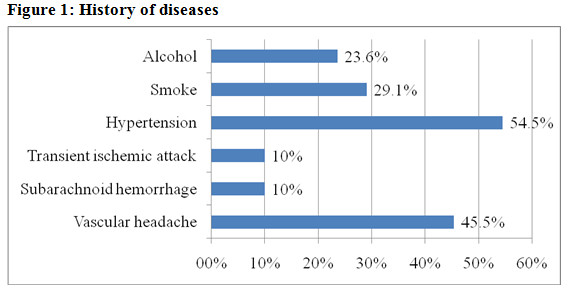
Vascular headache is an important symptom in clinical practice, especially in young people.
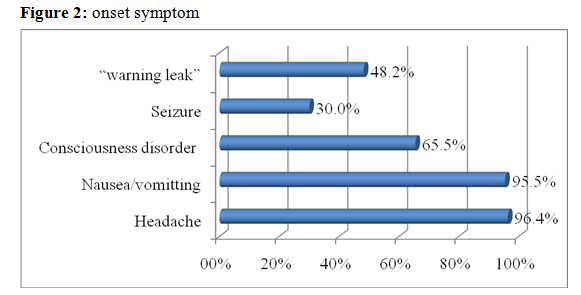
“warning leak” sign appeared in 48.2% (fig 2). According to Forsting M, Wanke I, Pearse Morris 50% patients have warning leak sign. They have severe headache, nausea and/or vomiting 1-2 weeks. The symptom may disappear spontaneously. So most of those patient did not be diagnosed.
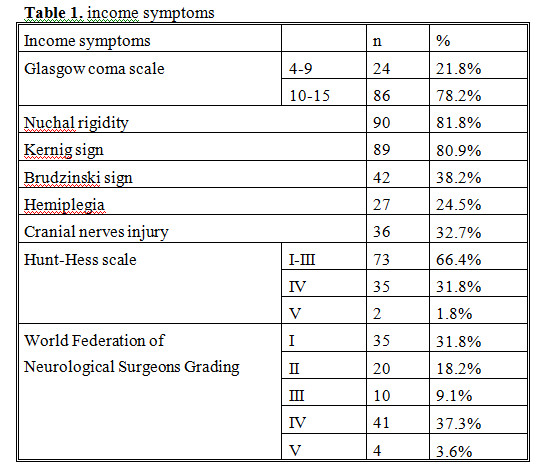
Most patients had Hunt-Hess scale I-III (66.4%). For more severe patients, we gave emergency aid first. Then we considered applying endovascular treatment if they became better.
Aneurysms characteristics

Most patients (86.4%) have 1 aneurysm.
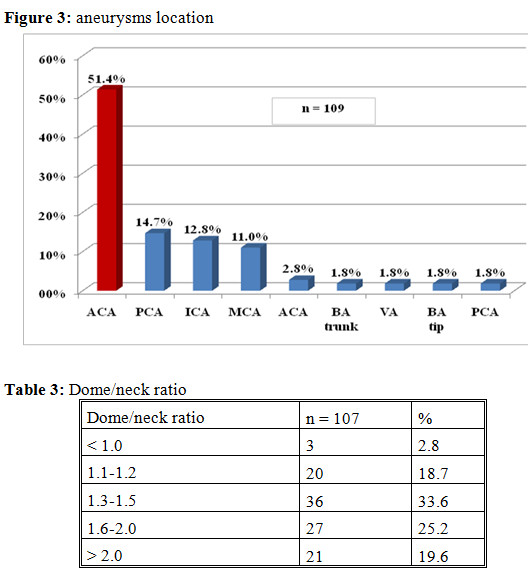
There were 62.6% aneurysms have narrow neck and 37.4 have wide neck.
Shape of aneurysms: saccular aneurysm 98.2%; fusiform aneurysm 1.8%.
Outcome
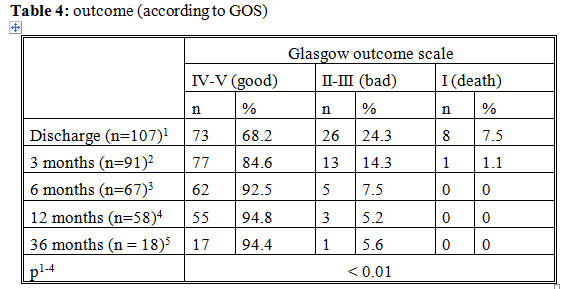
Good outcome at discharge 68.2%, after 12 months 94.8%. In a study of Dai Dinh Pham, mortality rate of patient who was treated by internal medicine only (without endovascular therapy) is 55.7%.
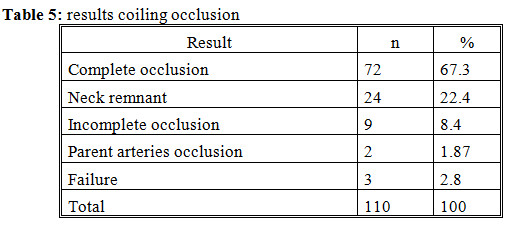
In a study of Pierot L (138 patients): complete occlusion 61.5%, neck remnant 33.2%, incomplete occlusion 5.3%. In study of Pierot L. on 138 patients: complete occlusion 61.5%; neck remnant 33.2%; incomplete occlusion 5.3%.
COMPLICATIONS
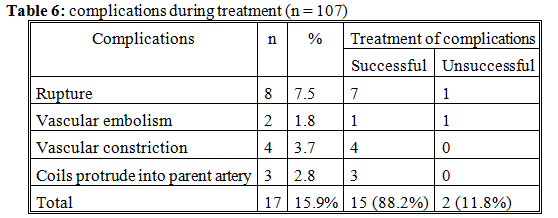
There were 15.9% patients manifest complications. We treated successfully for 88.2% of them.
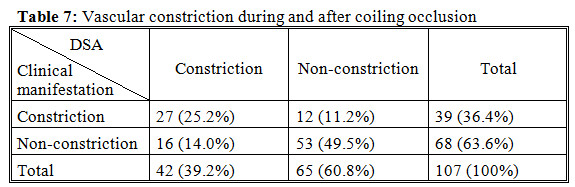
We detected 39.2% patients had vascular constriction on DSA but only 25.2% manifested clinical state of constriction.
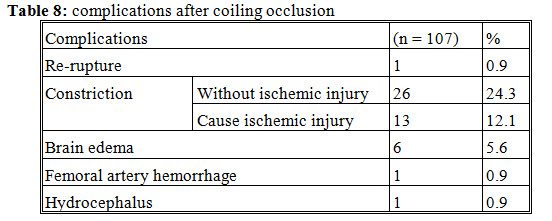

Constriction expressed in 36.4% patients and 12.1% of them had ischemic injury because of vascular constriction.
ANEURYSM RECURRENCE AFTER COILING
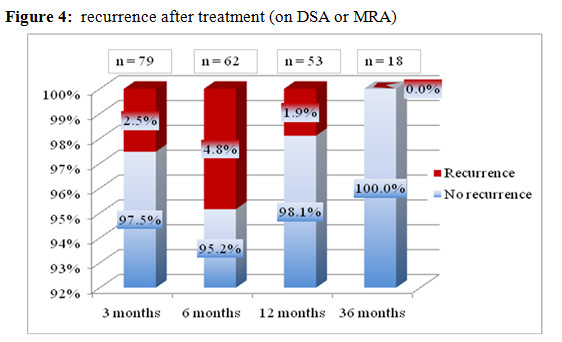
We detected recurrence on 2.5% patients after 3 months; 4.8 after 4.8 months and 0% after 36 months.
CONCLUSION
After studying on 110 intra-cerebral hemorrhage patients because of aneurysms rupturing at hospital 103 and Military central hospital 108 from June 2008 to April 2011 we had conclusions:
- History of disease: hypertension 54.5%; vascular headache 45.5%.
- Onset symptoms: “warning leak” 48.2%; nausea/ vomiting 95.5%; severe headache 96.4%.
- Popular location of aneurysms is in anterior communicating arteries.
- Outcome: Good outcome at discharge 68.2%, after 12 months 94.8%.
- Complications: There were 15.9% patients manifest complications. We treated successfully for 88.2%. Among 8 patients (7.5%) re-rupture during endovascular treatment, we treated successful for 7 patients.
References
- 1. Finucane F.M., Newell D.W., et al. (2006), “Cerebral aneurysms”, NEJM, 355, pp. 2703-2704.
- 2. Hanggi D. Turowski B. Beseoglu K., Yong M. Steiger H.J. (2008), “Intra-Arterial Nimodipine for Severe Cerebral Vasospasm after Aneurysmal Subarachnoid Hemorrhage: Influence on Clinical Course and Cerebral Perfusion”, Am J Neuroradiol, 29, pp. 1053-1060.
- 3. Joshua B., et al. (2009), “Guidelines for the Management of Aneurysmal Subarachnoid Hemorrhage of American Heart Association–American Stroke Association”, Stroke, 40, pp. 994.
- 4. McDougall CG, Spetzler RF, Zabramski JM, et al (2012), “The Barrow Ruptured Aneurysm Trial”. J Neurosurg:116:135–144.
- Meyers PM, Schumacher HC, Higashida RT, et al (2009). “Reporting standards for endovascular repair of saccular intracranial cerebral aneurysms”. Stroke. 40:e366.
- 6. Molyneux A., Kerr R., Holman R., et al. (2002), “International Subarachnoid Aneurysm Trial (ISAT) of neurosurgical clipping versus endovascular coiling in 2143 patients with ruptured intracranial aneurysms: a randomised trial”, Lancet, 360, pp. 1267-1274.
- 7. Pearse Morris. (2007), Practical Neuroangiography, Lipprincott Williams & Wilkins, Philadelphia USA, (Philadelphia. Baltimre, New York, London, Buenos Aires, Hong Kong, Sydney, Tokyo).
- Pierot L, Leclerc X, Bonafe A, Bracard S. (2008), “Endovascular treatment of intracranial aneurysms with Matrix detachable coils: midterm anatomic follow-up from a prospective multicenter registry”. AJNR Am J Neuroradiol.29:57– 61.
- 9. Schonfeld A.R., McMullen M.A. (2008), “Treatment of Brain Aneurysms”, Rdtech, 79, pp. 515-531.
Dinh Dai Pham; Phuc Duc Dang - from the Department of Stroke, Hospital 103, Hanoi, Vietnam